 Many clients seeking care for their substance use disorder also have co-occurring mental health disorders – and vice versa. Treating both types of conditions at the same time by providing quality integrated services is more effective than treating each disorder separately.
Many clients seeking care for their substance use disorder also have co-occurring mental health disorders – and vice versa. Treating both types of conditions at the same time by providing quality integrated services is more effective than treating each disorder separately.
Yet while integrated care has been increasingly prioritized, it remains an often elusive goal. An estimated 17 million adults in the United States live with co-occurring mental health (MH) and substance use disorders (SUD), yet only 5.7% of these individuals receive treatment for both disorders (NSDUH, 2020).
While the list of barriers to integrating SUD and MH services is long, providers remain interested in and committed to better serving this population, something evidenced by a group of Oregon SUD providers who signed up for a year-long Northwest ATTC intensive technical assistance project aimed at enhancing their programs’ capacity to serve clients with co-occurring disorders.
The project was divided into phases aligning with Gregory Aarons and colleagues’ EPIS model for implementing innovative practices:
 The Exploration phase involved securing leadership buy-in, assessing the programs’ existing co-occurring disorder services capacity using the Dual Diagnosis Capability in Addiction Treatment (DDCAT) Index, and providing a detailed summary report with program-specific recommendations for enhancing the level of integration.
The Exploration phase involved securing leadership buy-in, assessing the programs’ existing co-occurring disorder services capacity using the Dual Diagnosis Capability in Addiction Treatment (DDCAT) Index, and providing a detailed summary report with program-specific recommendations for enhancing the level of integration.Participating programs worked on a variety of change projects ranging from increasing mental health referrals, to matching treatment to stages of change for both MH and SUD conditions, to increasing the availability of co-occurring disorder group counseling.
For example, Grants Pass Treatment Center (ORTC, LLC) increased their identification of mental health needs and referral to MH services within the first thirty days of treatment from 14% to 72% by increasing collaboration and coordination with mental health agencies, adding MH screening, and increasing the focus on mental health issues in case consultations.
 The primary goal of this project was to improve co-occurring disorder services for clients by having program leaders engage in an intensive technical assistance process that combined the use of the DDCAT Index and the NIATx process improvement model.
The primary goal of this project was to improve co-occurring disorder services for clients by having program leaders engage in an intensive technical assistance process that combined the use of the DDCAT Index and the NIATx process improvement model.
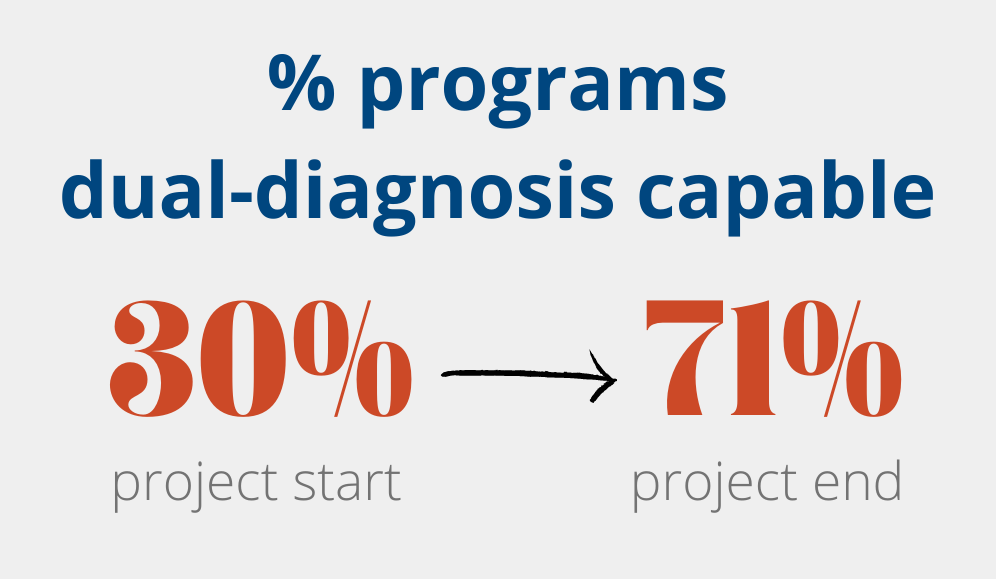
This goal was achieved with noteworthy results. The mean DDCAT score at the beginning (baseline) of the project was 3.21; this score had increased to 3.86 by the end of the project. Additionally, at baseline, just 30% of the programs were dual diagnosis capable, while at the final review, that figure had grown to 71%.
This suggests that future clients will be offered useful, integrated services to address their co-occurring MH and SUD challenges, a very exciting outcome for all involved.
The project's secondary goal was to collect qualitative data on the system-level barriers standing in the way of providers’ integration of care. This data was used by the Oregon Council on Behavioral Health to help advocate for additional funding to support integrated COD care. House Bill 2086 was passed by the Oregon legislature, allocating $10,200,000 in funding to support the development and implementation of payment structures/models that support integration of treatment and recovery support for individuals dealing with addiction and mental health diagnoses under one payment model.
Supporting the renewed interest in integration of MH and SUD services, this project provides a model for assisting programs to align policy, practice, and training efforts to support co-occurring disorder services.
Want to learn more about this project? Download our report.